Rosacea used to be called ‘acne rosacea’ yet it proves to be in stark contrast with acne vulgaris in manifestation and pathogenesis. There are red spots (papules) and sometimes pustules in both conditions, but in rosacea they are dome-shaped rather than pointed and there are no blackheads, whiteheads, deep cysts, or lumps. It mainly manifests itself as centrofacial erythematous macules with dilated capillaries with episodes of flushing due to vendodilation and inflammation. With chronicity edema will ensue as a result of vascular leakage and perivascular inflammation.
Rosacea may also result in reddened skin, scaling and swelling of affected areas. Pustules are larger in appearance, inflammatory and may contain pus. Skin flushing, dilated blood vessels and thickening of the skin in particular on and around the nose are often seen. Eye involvement is concurrently and frequently manifested. Acne inflammation may have a bacterial component to their makeup and are also mainly localized in and around the hair follicles.
Although it may first appear as early as the teen years, rosacea most frequently begins when sufferers enter their 30s, 40s or 50s affecting up to 10% of the population, as a flushing or transient redness on the cheeks or nose, and in some cases the chin or forehead. In this earliest stage, some patients may report stinging or burning sensations, including the feeling of dry or tight skin as opposed to acne patients who frequently complain of cutaneous oils.
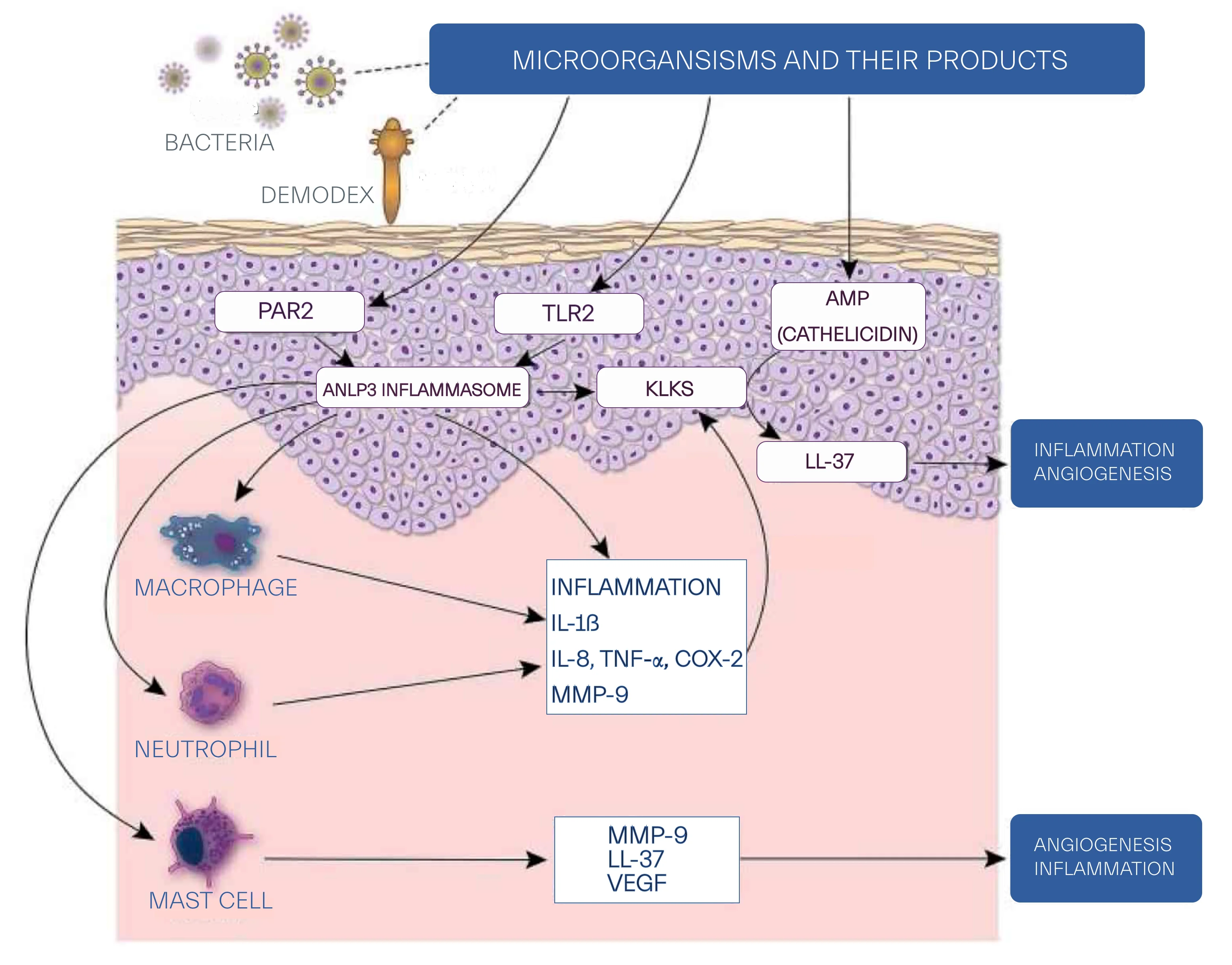
Overproduction of toll-like receptors and antimicrobial peptides has also been suggested as underlying mechanisms in pahogenesis of rosacea. Moreover, enhanced activity of cathlicidin, an antimicrobial peptide, augemented response of kallikreint-5, a serine protease, and neurovascular abnormalities have been proposed as pathophysiology of rosacea.
Studies indicate that sebum production does not change in rosacea patients and rosacea may not be linked to any skin type. Other studies found that while dry skin is seen more commonly in rosacea, sebaceous activity remains quantitatively unchanged. Sebum’s fatty acids concentration alters in rosacea with higher concentration for myristic acid as opposed to long chain saturated and mono unsaturated cis-11 eicosanoic fatty acids in lower quantities. All these studies support the use of rosacea skin care with provision of depleted fatty acids and other lost essential components of skin’s sebum.
Impaired skin barrier culminates in more exaggerated transepidermal water loss, TWE, which, in turn, more inflammation and hypersensitive skin. The skin of rosacea patients is more vulnerable to various skin care products as a consequence of increased TWE and increased penetrance of skin care ingredients into the skin. Therefore, the best rosacea skin care products address optimizing skin barrier function and restores transepidermal water loss.
Treatment options for rosacea, are quite distinct from treatment modalities for acne vulgaris, vary from non-pharmacological options to pharmacological ones based on severity and extent of the disease. Topical metronidazole has been found effective and routinely used as first line while azelaic acid has been demonstrated to be equally beneficial by restraining ROS generation and curbing pro-inflammatory cytokines implicated in rosacea.
A double-blind placebo control study randomized 31 rosacea patients to 320mg/day GLA, gamma linolenic acid, plus 100mg/day minocycline or placebo for 12 weeks assessed for erythema index and transepidermal water loss and stratum conrneum hydration and lipid concentration demonstrated significant superiority of GLA with p=0.033 and P=0.003. Another open label study of fourty four rosacea patients showed efficacy of 15% azalaic acid in a rosacea skin care routine with 1% dihydroavenanthramide D by a meaningful decline in investigator global assessment score and inflammatory lesions count. Tretinoids has been shown with equivocal results in various studies.
Use of plant extracts in treatment of rosacea
Various plant extracts have been studies for their anti inflammatory and vasoconstrictive effect, among them Potentilla erecta (L.) Raeusch , PE, is noteworthy for its tannins content and its inflammation-curbing impact as well as nitric oxide inhibitory effect comparable with those of corticoids. Agrimoniin content of PE was shown revealing not only curbing UVB-induced COX-2 expression but inhibitory effect to contain free radicals.
Disruption of the skin barrier is known as one of the fundamental culprits in pathogenesis of rosacea, which robustly suggest use of rosacea skin care in mild to medoerate cases and as maintenance treatment in severe disease. Specifically formulated for this chronic condition to enhance barrier function by mitigating inflammatory component, kallikrein 5 mediated, of rosacea as well as diminishing contact with environmental irritants. A skin care routine, aimed to restore the stratum corneum lipid barrier and to temper inflammation and vasodialation, of cleansing, moisturizing and sun protection is advocated by medical research.
It is of note, sun-induced COX-2 activation and PGE-2 expression leading to inflammation and vasodialation is a substantial piece in pathogenesis of rosacea, which brings to light importance of sun screen use in treatment of rosacea.
Bacterial dysbiosis is an inevitable aspect of rosacea pathogenesis and may be addressed in any product intended for rosacea treatment. While antibiotics most notably, metronidazole, receives good response and provide quick relief, its long-term effect and its contribution in shrinking remissions is under investigation and seems dubious.