Cystic acne presents a severe from of acne vulgaris and requires professional advice from a physician. They are rarely cancerous but addition of inflammation and bacteria through their rupture into the skin can render them painful and pus-discharging. Occasionally bacteria enter the cyst and cause an infection which resembles a boil. cysts are more likely to be associated with sequels and acne scars.
Severe cystic forms of acne may be manifestation of a systemic disease such as androgen excess and hormonal imbalance as in polycystic ovarian syndrome and warrants further medical investigation. It is of note that acne conglobata which presents with nodules and interconected cystic lesions with sinus tract, affecting trunk and limbs, is considered a severe and rare form of cystic acne.
In its differential diagnosis hidradenitis supurrative or acne inversa manifested with cysts and nodules on the body with sinus tract, may be considered. Acne inversa in its presentation and pathogenesis differs from acne vulgaris while proinflammatory cytokines are preeminently create a breeding ground for its development. Bacterial resistance to certain antibiotics and disruption of the skin microbiome are among other considerations in evaluating patients with severe acne.
Cystic acne should be consulted with a dermatologist. Small non-acneous cysts don’t usually require systemic treatment, but can be readily removed by a minor surgical procedure or managed using topical acne treatments. Larger ones are usually removed because they are unsightly or because they have been inflamed or can be medically managed.
Cysts are treated by making an excision in the skin. It is usually treated with isotretinoin and oral antibiotic, however, topical treatments may also be beneficial and sufficient in particular when body acne is not existent or considerable or may be used in conjunction with systemic treatment.
Some studies suggest use of carbon dioxide laser treatments combined with topical treatments for this type of acne to avoid systemic treatments and their adverse effects. Photodynamic therapy, PHT, has also been subject of multitude of studies which suggest PHT efficacy in treatment of mild to severe forms of acne. Moreover, cysts are more prone to development of acne sequels. Recurrence is not infrequent especially in case of initial treatment with isotretinoin.
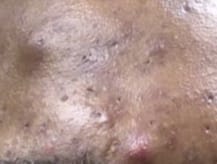
Manifestation of cystic acne
Nonpharmacologic treatments include: Gentle face washing, avoidance of manipulation of acne lesions. Oil-free products do not necessarily provide benefit and may stimulate further sebaceous secretions. Hypersecretion of sebaceous glands and sebum dysfunction in acne subjects render the skin depleted in essential fatty acids, which in turn further change acne microenvironment and result in a redundant excitement of sebaceous glands to produce sebum in excess .
PH-balanced cleansers containing essential fatty acids may correct this deleterious event. Salicylic acid preparations have been found helpful. Evidence-based skin care has gained a substantial role in management of mild to moderate acne as well as maintenance treatment of severe form of acne vulgaris.
Begin remedying with benzoyl peroxide gel in the morning. Add topical tretinoin or Adapalene in the evening. Add topical antibiotic such as erythromycin/clindamycin if not responsive to previous steps. Add systemic antibiotics such as tetracyclin, doxycycline, clindamycin, erythromyin.
If this form of acne is diagnosed, aforementioned steps could be circumvented and systemic agents such as oral isotretinoin can be directly initiated. This agent is associated with serious, dose dependent side effects which should be discussed in details with each patient in an effort to make a shared decision making. Combination therapy with benzoyl peroxide, doxycylcine and adapalen has been proposed to be superior to oral isotretinoin.
While above steps are taken during exacerbation of acne, topical treatment and evidence based acne skin care regimens find their significance in maintenance treatment armamentarium of this severe manifestation of acne. Acne skin care may be used initially in conjunction with oral therapy for optimal result and to avoid certain side effects associated with oral medications such as dry skin and atopic dermatitis. Topical therapy with oil free products may not be advisable as change in skin lipid composition occurs during the course of acne and should be addressed with proper skin care which provide to the skin essential fatty acids.